
Brandi was diagnosed with non-small cell lung cancer in 2018. Through advocacy and research, she's found treatment. However, she said, technology could make access to specialty medications easier.

Brandi was diagnosed with non-small cell lung cancer in 2018. Through advocacy and research, she's found treatment. However, she said, technology could make access to specialty medications easier.
In this digital version of the 2021 Medication Access Report: Complex Care & Specialty Medications Edition, we explore how patient-centric technology can help care teams and people needing specialty therapies take charge of their healthcare.
For a deeper dive into the specialty medication landscape, download the 2021 Medication Access Report: Complex Care & Specialty Medication Edition.
They say in times of crisis, you find out who your friends are.
But when Brandi Bryant was diagnosed with advanced-stage non-small-cell lung cancer at 39 years old, she didn’t wait for the fallout. She handpicked her support team.
“I need to build my team so that I can be ready for anything that comes next,” she said.

Brandi was diagnosed with non-small cell lung cancer in 2018. Through advocacy and research, she's found treatment. However, she said, technology could make access to specialty medications easier.

Brandi noticed shortness of breath after exercising that turned out to be effects of non-small cell lung cancer. After receiving the diagnosis, she rallied family and medical support teams.
With the ink still drying from the divorce papers she signed just before receiving her diagnosis, she decided to forge ahead as a single mother of four, without a partner.
She called her mom, who came in from Oklahoma to help take care of her and the kids.
She found a new oncologist — never returning to the doctor who delivered her diagnosis in a cold, robotic manner.
When she learned she also had the ALK biomarker, a gene expression that affects only 4 percent of lung cancers, she joined an ALK-positive lung cancer patient advocacy group.
And when her cancer progressed, she researched to find an ALK-positive lung cancer specialist for her care team.
Through treatments, side effects and the emotional burden she endured, Brandi never stopped working at her job as a production manager for a peer-reviewed journal. She said she likes to stay busy.
“I have a really great team that supports me, and they were able to back me up when I was barely sending emails,” Brandi said.
With a penchant for researching, Brandi learned all she could about her diagnosis and treatment options.
Originally diagnosed at stage 3b, she asked her oncologist about a targeted therapy available for ALK-positive lung cancer patients she’d heard about at a conference. Her oncologist pushed back and said her disease wasn’t advanced enough for the drug and insurance may not approve it. They were still hoping for curative treatment paths.
So, Brandi began chemotherapy and radiation.
But then she joined an online support group for ALK-positive lung cancer patients where she found encouragement and advice in speaking with other patients. She said if she had joined earlier, she may have pushed harder for answers on starting a targeted therapy, but instead went along with her doctor’s advice to stay the course in case insurance wouldn’t approve a more advanced or proactive approach.


Brandi found an online support group for her specific tumor type and biomarker. She's part of the growing percentage of patients who consult community support groups during treatment.
A couple months later, Brandi was admitted to the hospital for fluid buildup around her heart. When doctors drained and analyzed the fluid, they found malignant cells, advancing her diagnosis to stage 4.
Her oncologist said the tumor board at the hospital was split on prescribing targeted therapy or immunotherapy for stage 4 ALK-positive non-small-cell lung cancer. Brandi immediately knew she wanted the targeted therapy. She had read anecdotes in her support group that seemed to show immunotherapy wasn’t working well for patients with her diagnosis.
“I think that group saved me, I really do,” she said.
Recent research has shown ALK-positive lung cancer does not respond as well as other lung cancers to immunotherapy.Research Underway to Improve Immunotherapy Outcomes for ALK-Positive Lung Cancer, Lungevity, 2020
“My group knew that,” Brandi said.
Without Brandi digging into her own research and finding a support group, she may not have been as able to advocate for herself when the the care team was split on her therapy — a decision that clearly was going to be a significant shift in her outcome.
For patients prescribed specialty therapies, many support services exist to help navigate emotional, adherence and affordability challenges. While Brandi was proactive in finding support for her treatment plan and healthcare, many patients don’t have this support and don’t know where to find it. In one study, just 16 percent of patients were aware of services to help patients adhere to their therapy or treatment plan.Move The Needle: Amplifying the signal for patient services, Accenture, 2021 This means most patients navigate their treatment plan without support to understand their therapy options, managing side effects, care costs, time off work, maintaining therapy and, generally, how to cope.

While 63 percent of providers are aware of these support services, opportunities exist within integrated technology to help raise awareness and connect patients sooner.CoverMyMeds Provider Survey, 2019 Use of online and community patient resources have increased, but patients still most often consult their providers during treatment.Move The Needle: Amplifying the signal for patient services, Accenture, 2021
This is why it can be critical for providers to have answers and quickly surfaced resources, from medication-specific details to affordability programs, and even information about patient-relevant clinical trials, integrated within their EHR.
While the path to medication access for patients on specialty therapies is often non-linear, technology can help keep care teams connected. Solutions built with patients at the center can ensure connectivity of services in one place and provide visibility for the care team to help reduce complications and save time for more meaningful interactions.

After advocating for herself and researching her condition, Brandi was able to work with her care team to make an informed medication choice.
By the time Brandi was finally prescribed and started taking her targeted therapy, she could barely walk up a flight of stairs without losing her breath. The fluid they’d drained started to rebuild around her heart while she switched treatments, and the tumor in her lung continued to cause shortness of breath.
Within two weeks, however, she could fill her lungs with air again. As she described her experience after starting her medication, she savored a deep breath.
“It’s beautiful,” she said. “It’s gone. There’s nothing there.”
“Nothing” is the “something” many patients with cancer hope for.
Six weeks after starting her targeted treatment, she visited her oncologist for scans. Again, there was nothing. No evidence of disease. Though she had lingering effects from her 30 rounds of radiation, Bryant reveled in her progress. While it’s common for many specialty and oncology patients to try multiple lines of therapy, Brandi had no evidence of cancer in her body after only six weeks on her second line of therapy.
“I still had severe radiation esophagitis — I could not eat,” she said. “But I could breathe. I could breathe again.”

Medication management can be improved through interconnected, digital solutions that reduce manual methods such as phone calls and faxes.
Like many patients on specialty therapies, Brandi had to learn the best route of administration for her medication. She takes four large pills in the morning and four at night, which are best metabolized with a high-fat meal. As her caretaker when she first started taking her targeted therapy, Brandi’s mother was happy to oblige with large plates of eggs cooked with butter and cheese.
While her response to targeted therapy has been remarkable, managing her healthcare is an ongoing process, as Brandi juggles co-morbidities, ongoing doctor’s appointments and a full schedule of activities spread out among her four kids.
Her medication comes through the mail, and while Brandi says her pharmacy has an app, it doesn’t always work, which means she budgets time on the phone to call for refills, during which she often has to repeat her healthcare history.
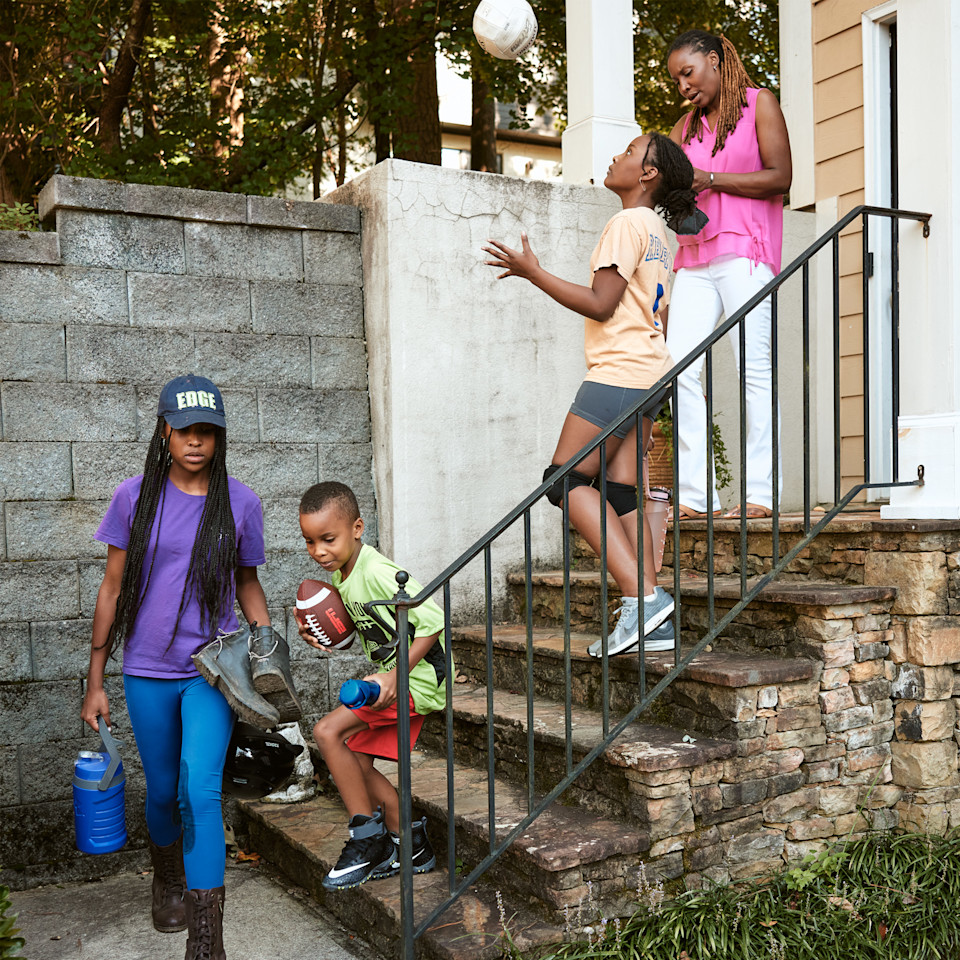
An interoperable healthcare system means Brandi and other people with chronic conditions can spend less time managing their care and invest more time on life's important moments — big and small.
While Brandi said she spends about 15 minutes on the phone for her refills, starting therapy for the first time can take much longer: 82 percent of patients report spending at least an hour to start specialty medications.CoverMyMeds Patient Survey, 2019 Over a third spend more than three hours on the phone, sharing information and asking questions among insurance companies, pharmacies and providers.CoverMyMeds Patient Survey, 2019
Brandi said she’d like everything about her care to be managed in one system, because even managing her medications alone is taxing.
Her plea to the healthcare industry?
“Please make things easier for patients,” Brandi said. “When people are feeling so bad, and you still have all of these obstacles that are impeding you just trying to get better … it’s distracting you from the ultimate goal of feeling the best you can.”
Information sharing through patient apps, portals and provider and pharmacy systems could alleviate not only the patient burden, but the care team administrative burden as well. In a recent survey, 81 percent of patients said they would support enabling various healthcare providers to electronically share patient health record information when they’re caring for the same patient.PEW HIT National Survey, PEW Charitable Trusts, 2020 This sharing could support true continuity of care and avoid exhausted patients having to fill in the blanks at each appointment.

After finding support in her care team and family, Brandi has resources in place so she can be present with her kids.
For Brandi, a lengthening health history — even if largely positive — is still a double-edged sword: Each new milestone, clear scan and checkup means she’s beating the odds of her diagnosis. But each new medication, test and set of appointment notes means she has a longer story to tell when ferrying information among pharmacies and providers.
“The whole healthcare system needs an update,” Brandi said. “I think they could use technology in a much better way. It would give me more time to just live my life, which is very precious.”
To read more about technology and industry trends surrounding specialty medications and prescribing, download the full 2021 Medication Access Report: Complex Care & Specialty Edition.

Sophia was diagnosed with Crohn's disease at 12 years old and barely remembers a life before daily medication, quarterly check-ups and annual scans and tests.
After graduating college during a pandemic and moving across the country, Sophia Garland started a new chapter of her life in summer 2021, complete with new responsibilities and her first full-time job.
She also took over full-time management of another project: Her chronic health condition and medications.
At 12 years old, Sophia was diagnosed with Crohn’s disease, an inflammatory bowel condition, after months of successive illnesses, including multiple bouts of strep throat and cold after cold. Her constant fatigue kept her from competing with friends on her swim team.
“My friends were starting to get really good, but I was losing all my muscle,” she said. “I would cry before going to swim practice, I hated it so much.”
Her condition took a year to finally diagnose. Sophia found that with the right medication, her Crohn’s disease was manageable, with little to no symptoms most days. She returned to swimming and life as a busy high school student, with an added track of doctor’s appointments and medication refills for her parents to keep up with.

Before Sophia started her first job out of college, her mother walked her through the steps of managing her prescriptions, arranging appointments and contacting their insurance.
After nearly a decade of serving as a caregiver and bookkeeper for her daughter’s various medications, labs, tests and appointments, her mom began to hand over the responsibilities during her last semester of college. Sophia started managing her own condition, including setting up doctor’s appointments, ordering medication refills and managing tests and scans.
“I didn’t realize how much she was doing until it was my turn to do it,” Sophia said. “It definitely gets confusing with all the different medications I’m on and trying to refill them because they go through different pharmacies.”
Patients managing one or two chronic conditions average six outpatient visits each year and nine prescription fills, with numbers increasing to correlate with the number of conditions each person has.Multiple Chronic Conditios in the United States, RAND Corporation, 2017

Sophia gets MRIs and colonoscopies on an annual basis and sees her gastroenterologist a few times a year. Because her Crohn’s symptoms are mild to unnoticeable much of the time, these regular appointments are especially important for her providers to understand if her current treatment is working. She’s switched medications at least twice based on test results.
“When I get MRIs and colonoscopies, they say (the effects of Crohn’s) are still an issue,” Sophia said. “That’s a weird balance for me because I feel fine but they’re telling me it’s not fine.”

Many patients liken starting, refilling and managing their specialty medications to a full-time job. For Sophia, these new responsibilities coincided with starting her first job out of college.
The bouts of physical illness Sophia has dealt with have come when complications arise with medication approval and access. After an appointment, her specialist decided to switch her medication, but several variables were at play: The specialist was in Missouri while Sophia was in Pennsylvania at college. Sophia’s specialist also prescribed more frequent dosing than what was standard for the medication.
Ultimately, approval took eight weeks because of the back-and-forth communications among the provider, insurance company, Sophia and the pharmacy. At one point, Sophia was without a medication for her condition entirely. Due to her unmanaged Crohn’s disease, Sophia ended up in the hospital for a week, diagnosed with Clostridioides difficile (C. diff), an Escherichia coli (E. coli) infection and mononucleosis.
Unfortunately, this storyline is common for patients prescribed specialty therapies. Inefficient processes of the specialty medication workflow can delay the start of treatment out to eight weeks, such as in Sophia’s case.The Impact of Disease-Modifying Therapy Access Barriers on People With Multiple Sclerosis: Mixed-Methods Study, Simacek et.al., 2018 During the interim period, patients have reported deteriorating health, worsening symptoms and disease progression.Move the Needle: Amplifying the Signal for Patient Services, Accenture, 2021
Care teams and patients can spend more than two weeks trying to resolve prior authorizations (PA) alone.2020 Medication Access Report, CoverMyMeds, 2020 Because most specialty medications require PA, technology that can automate PA processes and cut down turnaround time can help improve access and adherence for millions of patients.What is a prior authorization? CVS Specialty, 2021
More intricate electronic patient support solutions can provide visibility into the entire patient journey for providers and patients, spanning from enrollment to adherence, helping more patients access, afford and adhere to complex therapies by connecting stakeholders in one location.
For prescribers with this technology in place, patients receive therapy an average of 34 percent faster than the industry standard.CoverMyMeds data on file, 2020
“It’s definitely very frustrating,” Sophia said. “I think it’s hard for me to understand why my doctor is saying one thing, but (insurance is) saying no, and everyone I talk to … wants to help, but I’m on the phone in tears.”
If patients can overcome access challenges, affordability for specialty medications is often the next hurdle to starting therapy. When average annual costs for specialty therapies are $78,000 for one drug, it’s unfortunate, but not surprising, that patients are more likely to abandon specialty therapies than any other drugs during their insurance deductible period.Rx Price Watch Report: Trends in Retail Prices of Brand Name Prescription Drugs Widely Used by Older Americans, 2006 to 2020, AARP, 2021,Medicine Use and Spending in the U.S. A Review of 2017 and Outlook to 2022, IQVIA, 2018


Wrap-around services such as medication administration instruction and patient education programs can be critical to specialty medication adherence.
Sophia’s current medication costs over $12,000 for one dose, but thanks to a biopharma company savings program, it costs her no more than a cup of coffee per month. Direct connections to biopharma companies, integrated within provider and pharmacy software, can help patients learn about these savings opportunities sooner, helping them remain adherent to their medication.

While managing her medications may be new to Sophia, she’s a seasoned professional at administering her monthly injections. Many specialty medications, like Sophia's, cannot be taken by mouth, creating another layer of complexity for patients. As a teenager, Sophia learned to administer her own injections through a training session at the local children’s hospital.
Hub-connected services can provide additional support for patients, beyond simply affording and accessing their medication.
Through enrollment early in the specialty prescribing process, care teams, biopharma companies, payers and pharmacists can support patients with programs that include support for administration, treatment planning education and side effects and adherence. Patients even have the option for virtual injection training to help initiate therapy administration.
Care team members in these programs are specifically trained on drug-specific nuances of administration, treatment, side effects monitoring and additional program support for each specific therapy. In some cases, patients receiving behavioral coaching to support adherence for their medications are shown to be 25 percent more adherent and spend 31 more days on therapy.Symphony Health Analytics, 2016


In seasons of change, reliable, connected solutions can help those managing chronic and specialty conditions maintain control and transparency in their healthcare.
Within a few short months, Sophia moved into a new apartment, navigated a new city and started a new job. For many twenty-somethings, this is just learning the ropes of adulthood. Unlike her peers, though, she’s also learned in this time to navigate the pharmacy process for her specialty drug that requires refrigeration and administrative attention to detail.
If anything, she’s more prepared than ever for the challenges life will present.
“I’m definitely nervous for all these changes in my life, but I don’t think Crohn’s is something that’s holding me back from any of it,” she said.
To read more about care team and patient management of specialty medications, read the full 2021 Medication Access Report: Complex Care & Specialty Edition.
Press inquiries:
media@covermymeds.com
The Medication Access Report is developed in consultation with an advisory board of healthcare experts representing major organizations across the industry — each with unique perspectives, interests and opinions.